 By Dr John Nosti
By Dr John Nosti
A 50 year old patient called my office on a Thursday at 4:30pm (I close at 5pm) stating he had a front veneer come off and he would like to see me right away to fix it, he is currently 30 minutes from my practice and lives 2 hours from me (he was visiting the Jersey Shore for the weekend). He also says his mouth is a mess.
My first concern is “Do I wait around for this guy?”. Well, I am a nice guy and couldn’t let someone walk around without a front tooth. So I gambled and this gentleman walked in missing #10. I re-cemented it and discussed a few things.
Diagnostics:
Through my joint evaluation using Joint Vibration Analysis, I determined he had a “click” in his jaw and he indicated he used to be a boxer.
So #10 is recemented now (don’t crucify me on that one, you know the old analogy… filet mignon from chop meat). After I gave him my “heart to heart” with a little flare. I knew he was only “down for the weekend” (Jersey Shore lingo) so I talked to him like I was his best friend and told him to go back to see “his dentist” right away for some concerns.
Well, I wondered if I would see him back and low and behold he scheduled and shows up for his records appointment. We take a full set of records including joint history and Joint Vibration Analysis.
Have you ever wondered why some people click and it hurts and others click and it doesn’t? Have you ever wondered why some people come to your office and report that their jaw used to click, then it stopped, all this time not having pain, now it has started clicking again and their jaw hurts?
How does someone click, stop, then click again?
This may be basic TMD for some of you out there… for others this is something you may have chosen to ignore because you do not want “The TMD” practice. However, after doing a ton of rehabs, treating a ton of TMD patients, and equally important– being involved in a live patient Full Mouth rehab seminar for over 6 years I can tell you that very few people require a full mouth rehab due to breaking down their occlusion, without also tearing up their joints.
I will say that my restorative treatment plan does change depending on the disc displacement. MY end goal is always the same, but what happens in between does change.
Tx Planning:
To me this isn’t someone that has severe wear present. His canines are worn, and he has some erosive issues. He has had bicuspid extraction with retraction appliances and has the typically two step occlusion we often see in these post ortho cases.
If he was breaking teeth every so often it would concern me but he doesn’t report a history of breaking teeth. He told me a lot of his dentistry is old (including the maxillary veneers which I believe were >15 years old).
His primary concern is his appearance.

My next step here:
1. In office fabricated deprogrammer once the patient agrees to their records appointment.
2. Patient returns in 2 weeks for records wearing the appliance as follows
(patient is to wear the deprogrammer every night for a period of 2 weeks. The night before the records appointment the patient is to wear the appliance to bed and present to the office not having taken the deprogrammer out the night before.)
3. Diagnostic records are taken including upper and lower PVS impressions, Facebow, photos, and open bite record
(let’s call it modified CR bite, with a composite ball). If an increase in vertical is desired the modified CR bite is taken at
the desired vertical to be restored to.
4. For this patient lateral bites are taken, as well as protrusive bites and sent to the lab.
5. Final ceramic sizes, etc.. are dictated to the lab for wax-up.
So when I take records I take very accurate VPS impressions… not aliginates, for a wax-up.
What other records are you going to send to your lab (with the facebow and the VPS impressions)?
This patient was fed up with his appearance and literally asked what would it cost to have a complete mouth make-over. For my treatment plan, I presented a full mouth rehab 28 units of all ceramic restorations.
Of course the next question was how quickly could he have it done.
So my records that are done on cases like this would be:
1 JVA- completed
2 Facebow
3 VPS impressions of the top and bottom teeth
4 Deprogrammed CR bite
5 Lateral bites
6 Protrusive bite
7 Photos
 If this patient said he wanted things done quickly what would be your prep sequence?
If this patient said he wanted things done quickly what would be your prep sequence?
Would you prep top and bottom teeth at the same visit? Would you include the molars at the same visit? How would you control the bite through your prep sequence if you were opening vertical?
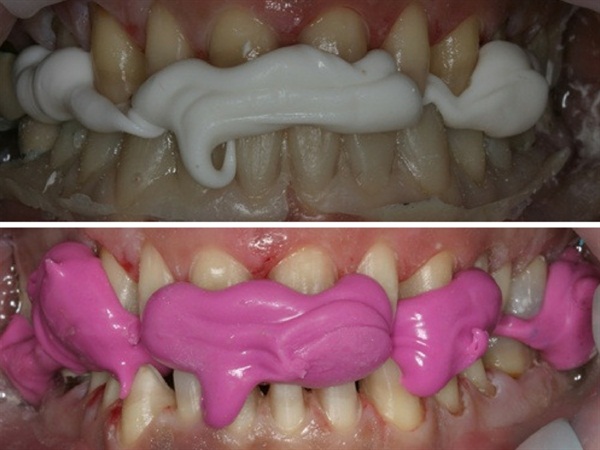
What I do is place my mock up in first and only reduce slightly to get this in over the patient’s existing teeth. The lab gives me a model that shows me where they needed to reduce to get the wax up done. You can prep through the mock up to make sure you have adequate reduction without over reducing!
Wax up done and now it is time to evaluate and place the mock up. Usually in full mouth rehabs there is very little pre-op reduction that is required to get the mock up in place. So we take the molar control bites (posterior CR bite registrations we took at the records appointment that is returned from the lab and we reconfirm our VDO). We then place the mock up and the molar control bites back into position.
We can then get the patient numb and start prepping. The mock up is used for depth guide cuts and reduction off of what the finals are going to look like. This way we have perfect reduction without over or under reducing. The main benefit is controlling the VDO and occlusion so that you can prep as you wish, stop and take a bite registration knowing that you are at your desired vertical dimension.
I know there is only one molar control bite in during this picture. If you were pr
epping bilaterally posteriors I would put both molar control bites in.
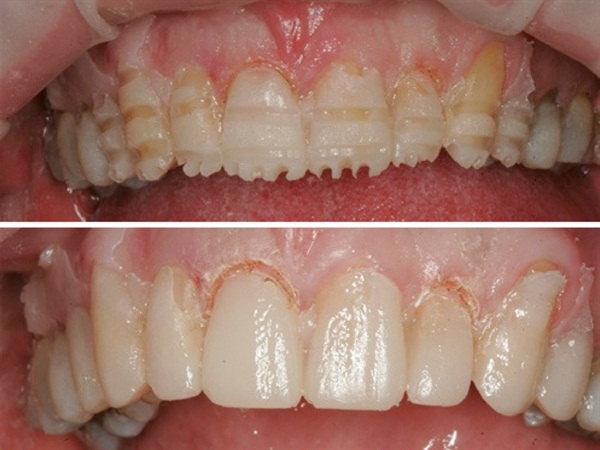
Prep the top ten and you have the bite. If you spot etch and bonded the lower overlay in you could clean up the flash and have them back at another time.
When we take the prep-to-prep view, I use Futar-D which sets very hard and can be trimmed with burs. You can be confident that the VDO you want will be held here at the prep to prep bite. So the patient is in temps for a few weeks while we wait for the ceramics to be fabricated.
This is when the rubber meets the road! When diagnosis and the case is set up properly, I don’t personally rely on the temporary phase to evaluate function, aesthetics etc. Those components should have been set up in diagnostics.So after 3 weeks and an interim appointment in my practice to equilibrate and refine aesthetic expectations, we schedule to cement upper and lower 10 units of e.Max by Gold Dust Dental Lab.



