Healthcare organizations are once again facing a familiar technology dilemma. Their Electronic Health Record systems helped digitize patient information, streamline documentation, and support clinical workflows. But healthcare technology expectations have changed dramatically over the last decade.
Today, hospitals and healthcare networks are expected to support real-time interoperability, advanced analytics, patient engagement platforms, remote care, and increasingly AI assisted decision support. These expectations are pushing many organizations to question whether their existing EHR systems are still capable of keeping up.
The immediate reaction in many boardrooms is straightforward. If the system feels outdated, perhaps it should simply be replaced.
However, replacing an EHR system is one of the most complex technology initiatives a healthcare organization can undertake. The cost, operational disruption, and implementation risks often force leaders to pause and reconsider.
Instead of asking whether the system should be replaced, many healthcare leaders are now asking a different question. Should we replace our EHR platform, or should we modernize the system we already have?
Understanding this distinction is critical for organizations planning their next phase of healthcare IT transformation.
Why Healthcare Organizations Are Reevaluating Their EHR Systems
The first generation of EHR platforms was designed primarily to digitize patient records and support billing workflows. These systems brought enormous improvements compared to paper-based processes. But they were not built for today’s interconnected healthcare environment.
Healthcare delivery has become increasingly dependent on data exchange between systems. Hospitals must share clinical data with external providers, laboratories, pharmacies, and health information exchanges. At the same time, new care models such as telehealth and remote monitoring require EHR platforms to connect with digital health applications and patient facing technologies.
Many healthcare organizations now operate dozens of systems across departments, each generating valuable clinical and operational data. When these systems cannot communicate effectively, clinicians may struggle to access a complete picture of patient care.
Interoperability has therefore become one of the most important drivers behind EHR modernization discussions. When data flows seamlessly between systems, clinical teams can coordinate care more effectively and reduce operational inefficiencies.
Improving connectivity between healthcare platforms is increasingly seen as a foundational step toward stronger healthcare operations. In fact, strengthening interoperability and integration across clinical systems can significantly improve how patient data moves across the healthcare ecosystem, as discussed in - The Power of EHR Integration to Level up Healthcare Operations.
As healthcare organizations continue expanding their technology landscape, the limitations of older EHR architectures become more visible.
What EHR Replacement Actually Means
When organizations consider replacing an EHR system, they are typically considering a complete transition from their current platform to a new vendor solution.
This process is far more involved than implementing new software. Healthcare organizations must migrate years of patient data, clinical documentation, billing records, and operational information into the new environment. Each integration with external systems must be rebuilt or reconfigured.
The operational impact can be significant. Clinicians must adapt to new user interfaces and workflows, while administrative teams must learn new processes for scheduling, documentation, and reporting.
Even with extensive planning and training, productivity often drops during the early stages of a new system rollout. Large scale EHR replacement initiatives frequently take multiple years to complete and require significant financial investment.
For these reasons, replacement projects are usually pursued when the existing platform cannot support the organization’s long-term technology strategy.
What EHR Modernization Looks Like Instead
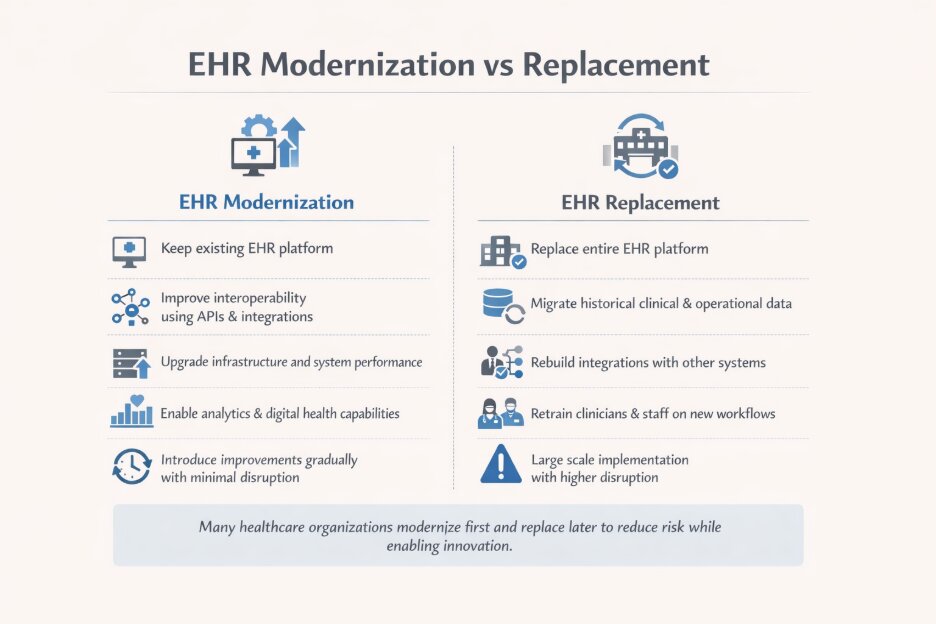
EHR modernization vs replacement healthcare strategy
EHR modernization offers an alternative path that focuses on improving existing systems rather than replacing them entirely.
Modernization strategies typically focus on upgrading infrastructure, improving interoperability, and introducing new capabilities around the existing EHR platform. Instead of rebuilding the entire system, organizations enhance their ability to connect with other technologies and support modern healthcare workflows.
For example, many modernization initiatives introduce integration layers that allow the EHR to exchange data through modern standards such as APIs and interoperability frameworks. These layers allow healthcare organizations to connect their EHR with analytics platforms, patient applications, and digital health tools without replacing the core system.
Modernization can also involve upgrading legacy infrastructure, improving system performance, and enabling cloud-based capabilities that support scalability and reliability.
This approach allows healthcare organizations to extend the life of their existing systems while still enabling innovation across clinical and operational environments.
Why Many Healthcare Leaders Choose Modernization First
For many healthcare organizations, modernization provides a more balanced approach to technology transformation.
One of the primary advantages is reducing disruption to clinical workflows. Physicians, nurses, and administrative staff can continue using the system they are familiar with while improvements are introduced gradually behind the scenes.
Modernization also allows organizations to adopt new technologies incrementally. Instead of waiting for a large replacement project to unlock new capabilities, healthcare organizations can introduce analytics platforms, data integration frameworks, and patient engagement tools step by step.
This gradual approach helps reduce implementation risks and allows leadership teams to prioritize investments based on operational impact.
Another important benefit is flexibility. By strengthening interoperability and integration capabilities, healthcare organizations can connect their EHR systems with emerging technologies more easily.
As healthcare continues moving toward data driven decision making, modernized systems can support analytics, population health management, and digital care platforms without requiring complete system replacement.
When Replacement Actually Becomes Necessary
While modernization can address many technology challenges, there are cases where replacing the EHR system becomes unavoidable.
If a platform is no longer supported by the vendor, maintaining security and reliability can become increasingly difficult. Some legacy systems were built on architectures that cannot support modern interoperability standards or integrate effectively with other healthcare technologies.
In these situations, replacement may be necessary to ensure long-term sustainability.
However, even when replacement becomes part of the long-term strategy, many healthcare organizations still pursue modernization initiatives first. Strengthening integration capabilities and improving infrastructure can stabilize the environment while organizations prepare for larger system transitions.
How Healthcare Leaders Should Approach the Decision
Choosing between modernization and replacement requires a strategic evaluation of both technology and organizational priorities.
Healthcare leaders must consider how well their current system supports interoperability, data integration, and future digital health initiatives. They must also evaluate the operational impact of large-scale system changes on clinical teams and patient care.
The decision ultimately depends on whether the existing system can evolve alongside the organization’s long-term digital strategy.
For many healthcare organizations, modernization provides an opportunity to unlock new capabilities while minimizing disruption. In other cases, replacement may be the best path forward when architectural limitations prevent meaningful system evolution.
Understanding the tradeoffs between these two approaches is essential for making informed decisions about the future of healthcare technology.
Discussions around EHR modernization services often emerge in this context, as healthcare organizations explore ways to extend the value of existing systems while preparing for future innovation. Modernization strategies can help organizations strengthen interoperability, support analytics, and improve system scalability without requiring immediate platform replacement.
As healthcare technology continues evolving, the most successful organizations will not necessarily be those that replace systems the fastest. They will be the ones who modernize thoughtfully, ensuring their technological environment can adapt to the changing demands of connected and data-driven healthcare.